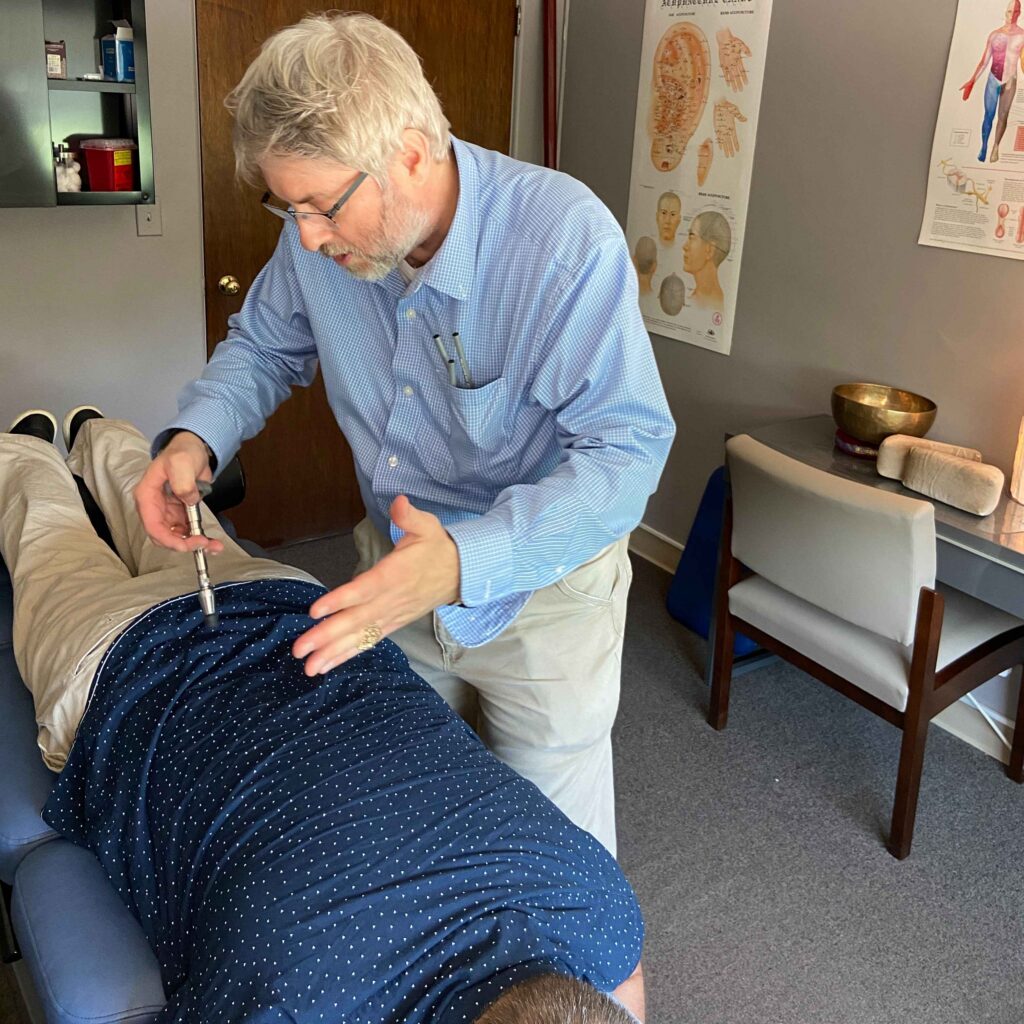
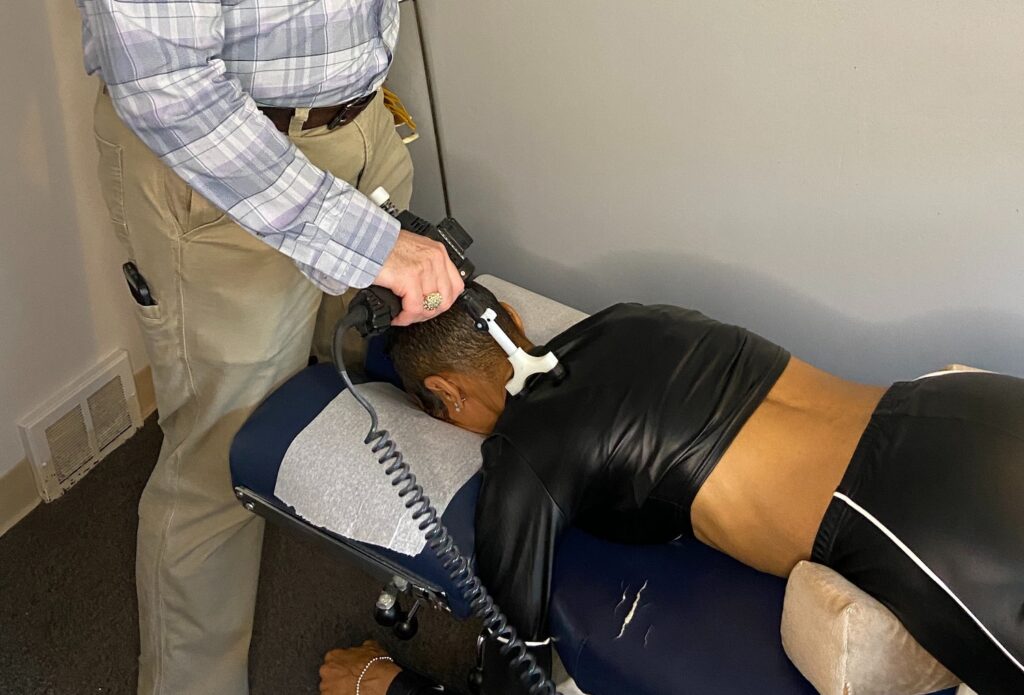
If you’ve ever felt a sharp, burning pain radiating down the back of your leg, you know how debilitating sciatica can be. This common condition affects millions of people every year, disrupting sleep, limiting mobility, and making even simple tasks like sitting or walking feel unbearable. Here in Lisle, IL, many patients who come to Northstar Integrated Health & Physical Medicine Center are searching for relief from sciatic nerve pain—and they’re often surprised to learn that the most effective approach doesn’t rely on just one type of treatment. Instead, combining chiropractic care with physical therapy offers a comprehensive, non-invasive solution that addresses both the underlying cause and the functional limitations sciatica creates.
At Northstar Integrated Health & Physical Medicine Center, we understand that sciatica isn’t a one-size-fits-all condition. Each patient’s experience is unique, shaped by different causes, severity levels, and lifestyle factors. That’s why our integrated approach brings together the expertise of chiropractors and physical therapists working side-by-side to create individualized treatment plans. This collaborative model has helped countless patients in the Lisle community reduce pain, restore function, and return to the activities they love—without surgery or long-term medication use.
What is sciatica? Sciatica refers to pain that radiates along the path of the sciatic nerve, which runs from your lower back through your hips and buttocks and down each leg. It’s typically caused by compression or irritation of the nerve roots in the lumbar spine, most commonly due to a herniated disc, spinal stenosis, or degenerative disc disease. The pain can range from a mild ache to a sharp, burning sensation, and may be accompanied by numbness, tingling, or muscle weakness in the affected leg.
Table of Contents
- Understanding Sciatica: More Than Just Back Pain
- Common Causes of Sciatic Nerve Pain
- Why a Combined Approach Works Better
- The Role of Chiropractic Care in Treating Sciatica
- How Physical Therapy Complements Chiropractic Treatment
- What to Expect During Integrated Treatment
- Recovery Timeline and Realistic Expectations
- Practical Tips for Preventing Sciatica Recurrence
- When to Seek Professional Care
Understanding Sciatica: More Than Just Back Pain
Sciatica is often misunderstood as simply “back pain,” but it’s actually a symptom of an underlying problem affecting the sciatic nerve. This nerve is the longest and thickest in the human body, roughly the diameter of your thumb. When compressed or irritated, it sends pain signals that can travel anywhere along its pathway—from your lower back all the way down to your foot.
The experience of sciatica varies considerably from person to person. Some describe it as an electric shock running down the leg. Others feel a constant, dull ache that intensifies with certain movements. Many patients report that the pain worsens when sitting for extended periods, which can make office work or long car rides particularly challenging. Here in Lisle, we frequently see patients whose sciatica began gradually—perhaps with occasional twinges—before progressing to more consistent, debilitating pain.
What makes sciatica especially frustrating is how it can affect one side of the body while leaving the other completely normal. This asymmetry can throw off your gait, create compensatory movement patterns, and lead to additional musculoskeletal problems if left untreated. The condition can also interfere with reflexes and cause noticeable weakness in the calf or foot muscles, making activities like climbing stairs or standing on tiptoe difficult.
Understanding that sciatica is a symptom rather than a diagnosis helps explain why treating just the pain—through medication alone, for example—often provides only temporary relief. The key to lasting improvement lies in identifying and addressing what’s compressing or irritating the nerve in the first place.
Common Causes of Sciatic Nerve Pain
Several different conditions can lead to sciatica, and identifying the specific cause is essential for developing an effective treatment plan. At Northstar Integrated Health & Physical Medicine Center, we conduct thorough evaluations to determine what’s triggering your symptoms.
Herniated or bulging discs are among the most common culprits. The cushioning discs between your vertebrae can weaken over time or become damaged through injury, causing the soft inner material to push outward and press against nerve roots. This typically occurs in the L4-L5 or L5-S1 segments of the lower spine, directly affecting the sciatic nerve pathway.
Spinal stenosis involves narrowing of the spinal canal, which can compress nerves as they exit the spine. This condition is more common in adults over 50 and often develops gradually as part of the natural aging process. Bone spurs, thickened ligaments, and degenerative changes all contribute to this narrowing.
Degenerative disc disease occurs when the spinal discs lose height and flexibility over time. As discs degenerate, the space between vertebrae decreases, potentially allowing bones to pinch nearby nerves. This process can also lead to instability in the spine, creating additional irritation.
Piriformis syndrome presents differently from other sciatica causes. In this condition, the piriformis muscle in the buttock becomes tight or spasms, compressing the sciatic nerve that runs beneath or through it. This is often seen in people who sit for long hours or engage in activities that overwork the hip muscles.
Spondylolisthesis happens when one vertebra slips forward over the one below it, potentially compressing nerve roots. This can result from degenerative changes, stress fractures, or structural abnormalities present from birth.
Less commonly, pregnancy, trauma from falls or accidents, tumors, or inflammatory conditions can also trigger sciatic symptoms. Each of these causes requires a slightly different treatment approach, which is why the comprehensive evaluation at our Lisle facility is so important.
Why a Combined Approach Works Better
Research increasingly supports what many healthcare providers have observed in practice: combining different conservative therapies often produces better outcomes than relying on a single treatment modality alone. When it comes to sciatica, the partnership between chiropractic care and physical therapy creates a powerful synergy that addresses multiple aspects of the condition simultaneously.
Chiropractic care excels at restoring proper spinal alignment and movement, reducing nerve interference, and improving overall biomechanics. Physical therapy focuses on strengthening supporting muscles, improving flexibility, correcting movement patterns, and building long-term resilience. Together, these approaches create a comprehensive treatment strategy that not only relieves current symptoms but also reduces the likelihood of recurrence.
Evidence from systematic reviews published in journals like Spine and the Journal of Manipulative and Physiological Therapeutics indicates that multimodal conservative care can be highly effective for managing sciatica. The combination approach allows practitioners to address both structural and functional issues, creating faster progress and more sustainable results.
At Northstar Integrated Health & Physical Medicine Center, this integrated model means you benefit from two sets of clinical expertise working toward the same goal. Your chiropractor and physical therapist communicate regularly about your progress, adjusting treatment protocols as you improve. This coordination eliminates the fragmented care that sometimes occurs when seeking treatment from separate, unconnected providers.
The combined approach also tends to be more efficient. Rather than trying one therapy for several weeks, evaluating results, then switching to something else if improvement is inadequate, you receive concurrent treatments that complement each other from day one. Many patients in Lisle report noticing meaningful improvement within the first few weeks of integrated care.
The Role of Chiropractic Care in Treating Sciatica
Chiropractic care offers several techniques specifically beneficial for sciatica sufferers. The foundation of chiropractic treatment involves carefully analyzing your spine to identify areas of restricted movement, misalignment, or dysfunction that may be contributing to nerve compression or irritation.
Spinal adjustments are performed to restore proper motion and alignment to vertebral segments. For sciatica patients, these adjustments often focus on the lumbar spine and pelvis, addressing the areas where nerve roots exit the spinal column. The goal isn’t to “pop a disc back into place”—that’s a common misconception—but rather to improve joint mechanics, reduce inflammation, and create an optimal environment for healing.
The type of adjustment used varies based on your specific condition and comfort level. Some patients respond well to traditional manual adjustments, while others may benefit from gentler techniques like flexion-distraction therapy. This specialized table-based technique uses gentle stretching motions to create space between vertebrae, reducing pressure on the disc and nerve without forceful manipulation.
Soft tissue work often accompanies spinal adjustments. Tight, spasmed muscles in the lower back, hips, and legs can perpetuate sciatic symptoms and limit the effectiveness of other treatments. Techniques like instrument-assisted soft tissue mobilization, trigger point therapy, and myofascial release help relax these muscles and improve tissue quality.
Chiropractors at Northstar Integrated Health & Physical Medicine Center also assess your pelvis and sacroiliac joints. Dysfunction in these areas can create asymmetry that affects sciatic nerve irritation. Gentle mobilization of the pelvis and SI joints often provides significant relief, especially in cases where piriformis syndrome contributes to symptoms.
Beyond hands-on treatment, your chiropractor provides education about posture, body mechanics, and positions that minimize nerve irritation. Many patients don’t realize that certain sitting positions or sleep postures can worsen sciatica. Simple modifications based on your chiropractor’s recommendations can accelerate healing between treatment sessions.
How Physical Therapy Complements Chiropractic Treatment
While chiropractic care addresses structural and alignment issues, physical therapy builds the strength, flexibility, and movement patterns necessary for lasting recovery. The physical therapists at Northstar Integrated Health & Physical Medicine Center design exercise programs tailored to your specific presentation of sciatica.
Therapeutic exercises form the cornerstone of physical therapy for sciatica. Early in treatment, exercises may focus on gentle nerve gliding techniques that help the sciatic nerve move more freely through surrounding tissues. These neural mobilization exercises can reduce irritation and improve symptoms without requiring intense exertion.
As you progress, strengthening exercises become increasingly important. The core muscles—including the deep abdominals, back extensors, and hip stabilizers—play a crucial role in supporting the spine and preventing excessive stress on discs and nerves. A weak core forces the spine to handle loads it wasn’t designed to bear, increasing injury risk.
Physical therapy also addresses muscle imbalances that commonly accompany sciatica. Many patients develop tightness in the hip flexors, hamstrings, and piriformis muscle, while simultaneously showing weakness in the glutes and core. This combination creates poor movement mechanics that perpetuate the problem. Targeted stretching and strengthening correct these imbalances.
Manual therapy techniques used by physical therapists complement chiropractic adjustments. Joint mobilization, soft tissue massage, and stretching all help improve flexibility and reduce muscle guarding. These hands-on techniques prepare your body to benefit maximally from therapeutic exercises.
Modalities like ice, heat, electrical stimulation, or ultrasound may be used judiciously to manage pain and inflammation, particularly in the acute phase of treatment. However, physical therapists emphasize active participation through exercise rather than passive treatments, as research consistently shows that active rehabilitation produces better long-term outcomes.
Physical therapists also provide detailed instruction on proper body mechanics for daily activities. Learning how to lift, bend, sit, and move in ways that protect your spine prevents re-injury and builds confidence in your body’s capabilities.
What to Expect During Integrated Treatment
When you begin integrated care at Northstar Integrated Health & Physical Medicine Center in Lisle, your treatment journey follows a structured yet flexible path designed around your individual needs and progress.
Initial evaluation involves comprehensive assessments from both your chiropractor and physical therapist. They’ll review your health history, discuss when and how your symptoms began, and perform orthopedic and neurological tests to identify the likely source of nerve irritation. Range of motion measurements, strength testing, and gait analysis provide baseline data to track your improvement.
Diagnostic imaging like X-rays or MRI may be recommended if your examination findings suggest the need for a clearer picture of spinal structures. These images help rule out serious pathology and guide treatment planning, but they’re not always necessary for every patient.
Treatment frequency typically begins with more frequent visits—often 2-3 times weekly—during the acute phase when pain is most intense. This allows for consistent hands-on care and close monitoring of your response. As symptoms improve, visit frequency gradually decreases, transitioning toward more independent exercise and maintenance care.
Each appointment may include elements from both chiropractic and physical therapy disciplines. You might receive a spinal adjustment followed by therapeutic exercises, or complete a strengthening circuit before soft tissue work. The exact combination evolves as your condition improves.
Communication between providers happens regularly at our facility. Your chiropractor and physical therapist discuss your progress, share observations, and adjust your treatment plan collaboratively. This coordination ensures everyone stays aligned on goals and timelines.
You’ll receive a home exercise program relatively early in treatment. Consistency with these exercises significantly impacts recovery speed and quality. Most home programs require just 15-20 minutes daily and include exercises you can perform with minimal or no equipment.
Recovery Timeline and Realistic Expectations
One of the most common questions patients ask is, “How long until I feel better?” The honest answer is that recovery timelines vary considerably based on several factors including the underlying cause, severity of nerve compression, duration of symptoms before seeking treatment, and individual healing capacity.
Many patients experience some degree of pain reduction within the first 2-3 weeks of integrated treatment. This initial improvement often comes from reduced inflammation, improved muscle relaxation, and better nerve mobility. However, complete resolution typically takes longer—often 6-12 weeks for moderate cases.
Acute sciatica that’s been present for just a few weeks generally responds faster than chronic cases that have persisted for months or years. Long-standing conditions often involve more tissue changes, muscle atrophy, and compensatory movement patterns that require more time to reverse.
The severity of nerve compression also influences recovery time. Mild compression causing primarily pain may resolve faster than severe compression that’s produced significant weakness or numbness. Cases involving structural issues like large disc herniations may require longer conservative care before substantial improvement occurs.
It’s important to understand that improvement rarely follows a straight line. You might have excellent days followed by temporary setbacks, especially as you become more active and begin challenging your body in new ways. These fluctuations are normal and don’t necessarily indicate treatment failure.
Research published in the British Medical Journal has shown that the majority of sciatica cases improve significantly with conservative care within 6-12 weeks. However, some degree of residual symptoms isn’t uncommon, and maintaining good spinal health through proper movement, exercise, and periodic wellness care helps prevent recurrence.
At Northstar Integrated Health & Physical Medicine Center, we set realistic expectations from the beginning and celebrate progress at every stage, whether that’s being able to sit through a meal without pain, walking farther without numbness, or returning to recreational activities you enjoy.
Practical Tips for Preventing Sciatica Recurrence
Successfully recovering from sciatica is a significant achievement, but preventing future episodes requires ongoing attention to how you use and care for your body. The habits you develop now can protect you for years to come.
Maintain core strength through regular exercise. Your core muscles stabilize the spine and pelvis, reducing excessive stress on discs and joints. Simple exercises like planks, bird dogs, and bridges performed 3-4 times weekly provide substantial protection. The physical therapy team at our Lisle clinic can design a maintenance program appropriate for your fitness level.
Practice proper lifting mechanics every single time you pick something up, regardless of weight. Bend at your hips and knees rather than your waist. Keep objects close to your body. Avoid twisting while holding weight. These principles apply whether you’re lifting a heavy box or picking up a dropped pen—repetitive poor mechanics eventually catch up with you.
Optimize your workspace ergonomics if you have a desk job. Your monitor should be at eye level, your chair should support your lower back’s natural curve, and your feet should rest flat on the floor. Take regular breaks to stand, stretch, and walk. Prolonged sitting compresses discs and can perpetuate sciatica risk.
Stay active with low-impact exercise like walking, swimming, or cycling. Regular movement promotes healthy disc nutrition, maintains flexibility, and keeps supporting muscles strong. Aim for at least 30 minutes of activity most days of the week.
Address tightness promptly through regular stretching. The hip flexors, hamstrings, piriformis, and lower back muscles commonly become tight and can contribute to recurrent sciatica. Spending 10 minutes daily on targeted stretches maintains flexibility.
Maintain a healthy weight to reduce excess load on your spine. Each pound of body weight translates to approximately four pounds of pressure on the lower back during certain activities. Even modest weight loss can significantly decrease spinal stress.
Choose supportive footwear and avoid high heels for extended periods. Poor footwear alters your gait and posture, creating compensatory stress patterns that travel up the kinetic chain to your lower back and pelvis.
Get adequate sleep on a supportive mattress. Your sleeping position matters too. Side sleeping with a pillow between your knees or back sleeping with a pillow under your knees helps maintain neutral spinal alignment throughout the night.
| Daily Habit | Protective Effect | Implementation Tip |
|---|---|---|
| Core strengthening exercises | Stabilizes spine, reduces disc pressure | Start with 10-minute sessions, 3x weekly |
| Proper lifting technique | Prevents acute disc injuries | Practice with light objects until automatic |
| Regular movement breaks | Prevents tissue stiffness and compression | Set hourly reminders to stand and stretch |
| Targeted stretching routine | Maintains flexibility, reduces muscle tension | Focus on hips, hamstrings, and lower back |
| Ergonomic workspace setup | Minimizes sustained poor postures | Adjust chair, monitor, and keyboard height |
When to Seek Professional Care
Understanding when sciatica warrants professional evaluation helps you get appropriate care at the right time. While many cases of mild sciatic pain resolve on their own with rest and basic self-care, certain situations call for prompt professional attention.
Seek care soon if you experience sciatic pain that persists beyond a few days despite rest and over-the-counter pain relievers. Early intervention often leads to faster recovery and prevents the condition from becoming chronic. Many patients wish they’d sought treatment sooner after experiencing weeks or months of unnecessary suffering.
Immediate evaluation is warranted if you notice progressive weakness in your leg or foot, especially if it’s interfering with normal walking or causing foot drop. Significant weakness can indicate substantial nerve compression that may require urgent intervention.
Seek prompt care if you develop bowel or bladder dysfunction alongside back and leg pain. This combination could indicate cauda equina syndrome, a rare but serious condition requiring emergency medical attention. While uncommon, recognizing this red flag can prevent permanent complications.
Don’t delay care if your pain becomes severe enough to significantly limit daily activities like dressing, bathing, or performing essential job duties. Quality of life matters, and you don’t need to simply endure debilitating pain when effective conservative treatments are available.
Consider professional evaluation if you’ve had sciatica before and it’s returning, especially if episodes are becoming more frequent or severe. Recurrent sciatica often indicates underlying issues that need addressing beyond just symptom management.
Get assessed if you’re over 50 and experiencing sciatica for the first time, particularly if accompanied by unexplained weight loss or a history of cancer. While most sciatica in older adults stems from degenerative changes, ruling out serious pathology provides peace of mind.
At Northstar Integrated Health & Physical Medicine Center, we welcome patients at any stage of sciatica—from recent onset to chronic, long-standing cases. Our integrated approach adapts to wherever you are in your journey, providing appropriate care whether you need intensive initial treatment or guidance managing occasional flare-ups.
Myths vs. Facts About Sciatica Treatment
Myth: Bed Rest is the Best Treatment for Sciatica
Fact: While severe pain might require a day or two of limited activity, prolonged bed rest actually delays recovery. Gentle movement and appropriate exercise, guided by healthcare professionals, promote healing by maintaining circulation, preventing muscle atrophy, and reducing stiffness. Research consistently shows that staying reasonably active within pain tolerance leads to better outcomes than extended rest.
Myth: Sciatica Always Requires Surgery
Fact: The vast majority of sciatica cases improve with conservative treatment approaches like the integrated chiropractic and physical therapy model used at Northstar Integrated Health & Physical Medicine Center. Evidence indicates that 80-90% of patients experience significant improvement without surgical intervention. Surgery is typically considered only after extensive conservative care has been unsuccessful or when serious neurological deficits are present.
Myth: Once Your Sciatica Improves, You’re Cured Forever
Fact: While many people fully recover from sciatica episodes, the underlying factors that contributed to the condition may persist without proper management. Maintaining core strength, practicing good body mechanics, staying active, and addressing biomechanical issues through periodic wellness care significantly reduce recurrence risk. Think of sciatica recovery as establishing a healthier relationship with your spine rather than a one-time cure.
Myth: Chiropractic Adjustments Can Damage Your Spine
Fact: When performed by licensed, trained chiropractors, spinal adjustments are remarkably safe. Serious complications are extremely rare—far less common than risks associated with long-term medication use or surgical procedures. Chiropractors undergo extensive training in spinal biomechanics and assessment, and they modify techniques based on individual patient presentations to ensure safety and comfort.
Myth: You Can’t Exercise When You Have Sciatica
Fact: While certain activities may need temporary modification during acute pain, appropriate therapeutic exercise is essential for recovery. The key is choosing the right exercises at the right time. Physical therapists specialize in determining which movements will help rather than harm, progressively building your capacity as symptoms improve. Movement is medicine for sciatica when properly prescribed and progressed.
Final Thoughts from Northstar Integrated Health & Physical Medicine Center
Living with sciatica can feel isolating and overwhelming, but you don’t have to navigate it alone. Here in Lisle, IL, the team at Northstar Integrated Health & Physical Medicine Center is committed to helping you understand your condition, participate actively in your recovery, and build long-term resilience against future episodes.
The integration of chiropractic care and physical therapy represents more than just two treatments happening under one roof—it’s a coordinated, evidence-informed approach that addresses your sciatica from multiple angles simultaneously. This collaborative model has helped countless patients in our community reduce pain, restore function, and return to activities they thought they might have to give up forever.
Every patient’s journey with sciatica is unique, shaped by individual anatomy, lifestyle, and goals. What works beautifully for one person may need adjustment for another. That’s why personalized care, thorough evaluation, and ongoing communication between you and your healthcare team are so important.
If you’re experiencing sciatic nerve pain, know that effective, non-surgical options exist. The combined expertise available at Northstar Integrated Health & Physical Medicine Center provides a comprehensive pathway toward recovery—one that empowers you with knowledge, supports you with expert care, and equips you with tools for long-term spinal health.
Your spine carries you through every moment of every day. Investing in its health through proper care when problems arise isn’t just about reducing pain—it’s about protecting your ability to live actively, work productively, and enjoy life fully for years to come.
Frequently Asked Questions
How long does it take for sciatica to respond to combined chiropractic and physical therapy treatment?
Most patients notice some improvement within 2-3 weeks of starting integrated treatment, though complete resolution typically takes 6-12 weeks depending on severity and duration of symptoms. Acute cases generally respond faster than chronic sciatica, and individual factors like overall health and adherence to home exercises significantly influence recovery speed.
Can sciatica be treated without medication or injections?
Yes, many sciatica cases improve significantly with conservative care including chiropractic adjustments, physical therapy exercises, and lifestyle modifications. Research indicates that the majority of patients achieve meaningful relief through non-pharmaceutical approaches. While some patients use over-the-counter pain relievers temporarily, the goal of integrated treatment is to address underlying causes rather than just masking symptoms.
Is it safe to receive chiropractic adjustments if I have a herniated disc causing sciatica?
Chiropractors are trained to assess disc-related conditions and modify treatment techniques accordingly. Many herniated disc patients benefit from gentle approaches like flexion-distraction therapy rather than traditional high-velocity adjustments. Your chiropractor will perform a thorough evaluation and choose the safest, most appropriate techniques for your specific condition.
Will I need to continue treatment forever once I start?
No. The goal of integrated treatment at Northstar Integrated Health & Physical Medicine Center is to resolve your acute symptoms and equip you with knowledge and exercises to maintain spinal health independently. Treatment frequency decreases as you improve, eventually transitioning to occasional wellness visits if desired. Many patients successfully manage their spinal health long-term through the home exercise programs and self-care strategies learned during active treatment.
What’s the difference between chiropractic care and physical therapy for sciatica?
Chiropractic care focuses primarily on spinal alignment, joint function, and nervous system optimization through hands-on adjustments and mobilization. Physical therapy emphasizes therapeutic exercise, functional movement training, and building strength and flexibility. Both disciplines include manual therapy and patient education, but their primary emphasis differs, which is why combining them creates such comprehensive care.
Can sciatica come back after successful treatment?
Sciatica can recur if the factors that contributed to the original episode aren’t adequately addressed. However, patients who maintain core strength, practice proper body mechanics, stay active, and address early warning signs typically experience fewer and less severe recurrences. The education and preventive strategies provided during integrated treatment significantly reduce recurrence risk compared to symptom-only approaches.
TL;DR – Key Takeaways
- Sciatica results from compression or irritation of the sciatic nerve, commonly caused by herniated discs, spinal stenosis, or piriformis syndrome, and creates pain radiating down the leg along with potential numbness and weakness.
- Combining chiropractic care and physical therapy addresses both structural issues and functional limitations simultaneously, creating faster, more comprehensive results than single-modality treatment approaches.
- Chiropractic adjustments restore spinal alignment and joint function while physical therapy builds strength, flexibility, and proper movement patterns essential for long-term recovery and prevention.
- Most sciatica cases improve significantly within 6-12 weeks of integrated conservative care without requiring surgery or long-term medication use, though individual timelines vary based on severity and chronicity.
- Preventing recurrence requires maintaining core strength, practicing proper lifting mechanics, optimizing ergonomics, staying active, and addressing early warning signs before they develop into full episodes.