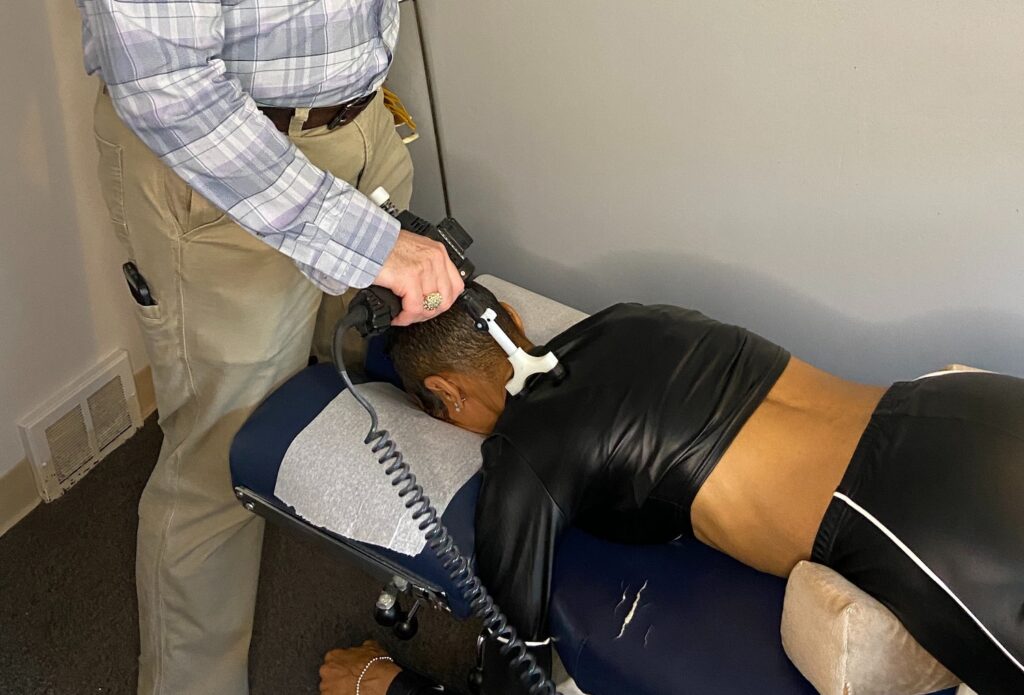
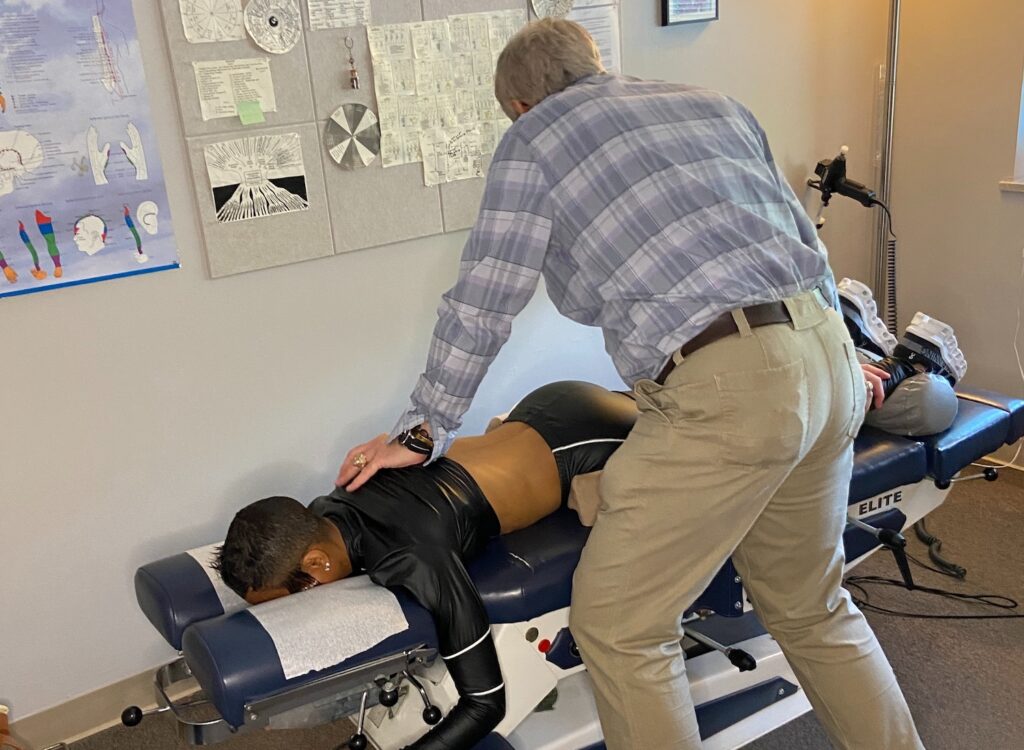
Stress-Related Headaches: How Chiropractic Care in Lisle Can Help
Stress and headaches often show up together. If you live or work here in Lisle, you may notice that a busy workweek, tight deadlines, or even a tough commute can leave your head pounding. As chiropractors at Northstar Integrated Health & Physical Medicine Center, we see this pattern every day. The good news: when you understand why stress triggers headaches, you can take practical steps to calm them—and chiropractic care can be a key part of that plan.
Why does stress trigger headaches? Stress sets off a chain reaction in your body—tightening muscles in your neck and shoulders, changing breathing patterns, impacting sleep, and increasing sensitivity in the nervous system. Together, these changes can spark or worsen headaches, especially tension-type and neck-related (cervicogenic) headaches.
Table of Contents
What Do We Mean by Stress-Related Headaches?
“Stress headache” is a common way people describe pain that ramps up with emotional or physical stress. Most often, this refers to tension-type headaches or headaches that start in the neck and radiate into the head (cervicogenic headaches). Migraines can also be influenced by stress, acting as a trigger in some individuals. The underlying drivers include muscle tension, joint irritation in the neck, changes in sleep, and increased nervous system sensitivity.
How Stress Triggers Headaches: The Brain–Body Connection
Stress is not just a feeling. It’s a whole-body response. Your brain signals the body to prepare for “fight or flight.” Muscles brace. Breathing changes. Sleep and digestion can be affected. Over time, these changes may set the stage for headaches.
When you’re stressed, the muscles at the base of your skull, along your neck, and across the shoulders often tighten. This can strain the small joints in the neck and irritate nearby nerves. It can also sensitize pain pathways that send signals into the head, creating that classic band-like pressure or pain behind the eyes.
Stress also affects posture. Long hours on a laptop, phone, or two monitors can slide you into a forward head position. That posture increases the load on the neck and upper back. Even a small forward head shift adds significant strain to the cervical spine. Over hours and days, that added strain often becomes a headache.
Other stress-related factors play a role too: jaw clenching, shallow breathing, caffeine swings, missed meals, and poor sleep. Many of our patients in Lisle tell us their headaches are worse during busy seasons, when they combine tight deadlines with less movement, more screen time, and skipped self-care.
Common Stress-Related Headache Types and What They Feel Like
Different headaches behave differently. Here’s a simple overview of common types we see and how stress can influence them.
| Headache Type | Typical Features | How Stress Plays a Role | Where Chiropractic May Help |
|---|---|---|---|
| Tension-type | Dull, pressure-like pain; often both sides; mild-to-moderate; may feel like a “tight band” | Increases muscle tension, promotes poor posture, disrupts sleep | Improve neck and mid-back mobility; reduce muscle tension; posture and movement coaching |
| Cervicogenic (neck-related) | Pain starts in neck/occiput and can travel to the head; often one-sided; neck stiffness | Amplifies neck muscle guarding and joint irritation | Targeted cervical and thoracic care; soft-tissue work; corrective exercises |
| Migraine | Throbbing or pulsating; often one-sided; sensitivity to light/sound; nausea; may have aura | Acts as a trigger in some; affects sleep, hydration, and routine | Address neck tension and triggers; co-manage with your medical provider as needed |
How Chiropractic Care May Help (Our Lisle Perspective)
Chiropractic care focuses on the spine, joints, muscles, and nervous system. For stress-related headaches, we look closely at the neck (cervical spine), upper back (thoracic spine), ribs, shoulder mechanics, and jaw habits. We also consider daily routines—your workstation setup, driving posture on I-88, and how you recover after long days.
A typical care plan is individualized. Our integrated clinic keeps chiropractic at the forefront while coordinating other supportive therapies when helpful. Here’s how we approach it:
- Thorough assessment. We begin with a detailed history and exam to determine whether your headaches are more tension-type, cervicogenic, migraine, or mixed. We screen for red flags and collaborate with medical providers when appropriate.
- Gentle, targeted spinal adjustments. When indicated, adjustments can help restore normal joint mechanics in the neck and upper back. Better mobility often reduces local irritation and tightness that contribute to headaches.
- Soft-tissue therapies. Muscle tension is a major player in stress-related headaches. Myofascial release, trigger point work, and instrument-assisted techniques can reduce muscle guarding in the suboccipitals, upper trapezius, levator scapulae, and jaw muscles.
- Posture and ergonomic coaching. Small workstation changes make a big difference. We address monitor height, chair support, keyboard reach, and how to alternate sitting and standing. We also coach on driving ergonomics for our commuters in and around Lisle.
- Corrective exercise. Simple home exercises help stabilize your gains. We focus on deep neck flexor activation, scapular control, thoracic mobility, and breathing drills that downshift a stressed nervous system.
- Integrated options. Depending on your needs, we can coordinate massage therapy, physical rehabilitation, acupuncture, or nutrition counseling within our integrated setting. Many patients benefit from a combined, conservative approach that reduces triggers from multiple angles.
- Evidence perspective. Research suggests that spinal manipulation and manual therapies can help with neck-related headaches and may reduce frequency or intensity in some tension-type or migraine cases. Results vary by individual. Our commitment is to conservative, evidence-informed care tailored to you.
Practical Ways to Reduce Stress-Triggered Headaches at Home
Small, consistent habits go a long way. Here are simple steps we often recommend in the clinic:
- Move every 30–60 minutes: stand up, roll your shoulders, gently tuck your chin, and breathe slowly for 60–90 seconds.
- Relax your jaw: keep teeth slightly apart and tongue resting on the roof of your mouth; consider a warm compress at the temples or jaw.
- Reset posture: set your monitor at eye level, keep elbows near your sides, and support your lower back.
- Hydrate and fuel: steady water intake and regular meals help reduce headache triggers for many people.
- Mind your caffeine: too much or too little can backfire; stay consistent and avoid late-day stimulants.
- Sleep routine: aim for a regular schedule, a cool dark room, and a wind-down ritual without screens.
- Practice 4–4–6 breathing: inhale 4 seconds, hold 4, exhale 6; repeat for 2–3 minutes to calm stress response.
- Heat or cold: warm shower for tight muscles or a cool pack at the base of the skull for 10–15 minutes as needed.
When to See a Chiropractor in Lisle
If your headaches are frequent, limiting your daily life, or clearly tied to neck and shoulder tension, a chiropractic evaluation is reasonable. Many people benefit when:
- Headaches have lasted more than a couple of weeks despite self-care.
- You notice stiffness, pain, or “knots” in the neck and upper back.
- Workstation time or driving reliably brings on symptoms.
- Over-the-counter medications are needed more than occasionally.
- You prefer a conservative, non-drug approach to reduce frequency or intensity.
Chiropractors are trained to evaluate musculoskeletal contributors, provide hands-on care, guide exercise and ergonomics, and coordinate care with other providers when needed.
When to Seek Medical Care Urgently
Most headaches are not dangerous, but some need prompt medical evaluation. Seek urgent care or call emergency services if you have a sudden, severe “worst headache of your life,” new neurologic symptoms (weakness, numbness, confusion, trouble speaking, vision loss), fever with neck stiffness, a headache after a head injury, or a new or changing headache pattern if you are pregnant or have a known medical condition that raises risk. If you’re unsure, err on the side of caution and seek medical advice.
Common Mistakes We See Locally
- Relying only on pain relievers. Medications can be helpful, but frequent use may lead to medication-overuse headaches. Conservative care and trigger management are important.
- Ignoring workstation strain. Between remote work and office time around Lisle, ergonomics matter. Monitor height, chair support, and keyboard placement often need small tweaks.
- Weekend catch-up without warm-up. Yardwork, home projects, and sports after a sedentary week can overload tight muscles. A few minutes of mobility work first helps.
- Skipping meals and hydration. Busy days and variable weather can amplify headaches for some people. Build steady routines to keep triggers predictable and fewer.
Myths and Facts About Stress, Headaches, and Chiropractic Care
- Myth: If stress causes my headaches, I just need to relax more. Fact: Relaxation helps, but mechanical factors—neck mobility, posture, and muscle tension—often need direct attention too.
- Myth: All headaches are the same. Fact: Tension-type, cervicogenic, and migraine headaches behave differently and respond best to an individualized plan.
- Myth: Chiropractic adjustments “cure” headaches. Fact: Chiropractic care can reduce mechanical contributors and help many people feel and function better. It’s not a cure-all and works best alongside healthy habits and, when needed, co-management.
- Myth: If I start chiropractic, I’ll have to go forever. Fact: Care plans should be goal-focused. Many patients see us more often initially, then taper to self-care with occasional check-ins as needed.
What to Expect at Your First Visit
We begin with a conversation about your headaches—when they started, where they hurt, what makes them better or worse, and your daily routines at work and home. We’ll ask about sleep, stress, hydration, and diet patterns because they can influence symptoms.
Your musculoskeletal exam may include posture assessment, neck and upper-back mobility testing, muscle tension evaluation, and neurologic screening if indicated. If we suspect non-musculoskeletal causes or red flags, we’ll refer you appropriately.
Treatment often starts the same day if appropriate. Many patients receive a combination of gentle spinal adjustments, soft-tissue work, and guided exercises. We’ll outline a clear plan that fits your goals, schedule, and comfort level. You’ll leave with practical steps to start reducing triggers right away.
Final Thoughts for Our Lisle Community
Headaches tied to stress are common, but you’re not stuck with them. With the right blend of hands-on care, movement, ergonomic updates, and simple daily habits, many people notice fewer and lighter headaches. Here in Lisle, our team at Northstar Integrated Health & Physical Medicine Center is dedicated to conservative, evidence-informed care that keeps chiropractic at the core and brings in other supportive therapies when they’re helpful.
If stress is driving your headaches, we’re here to help you create a clear plan—one that addresses your unique triggers and fits your life.
FAQs
How can I tell if my headache is from my neck?
Neck-related headaches often start at the base of the skull and can travel to the temples, forehead, or behind one eye. You may notice neck stiffness or that certain neck positions trigger pain.
Can chiropractic help with migraines, or only tension headaches?
Chiropractic care can help address neck and muscle tension that may trigger or worsen migraines for some people. It’s not a cure for migraines, but it can be part of a broader management plan.
Are chiropractic adjustments safe for headache patients?
When performed by a licensed chiropractor after an appropriate evaluation, spinal manipulation is generally considered safe for most people. We screen for risks and tailor techniques to your comfort.
How many visits will I need?
It varies. Many patients notice change within a few visits. Plans depend on your goals, how long the headaches have been present, and contributing factors like posture or muscle tension.
Will I need imaging for my headaches?
Most headache cases don’t require imaging. If your history or exam suggests something unusual, we’ll discuss appropriate referral or testing.
What if I’m pregnant or an older adult?
We adapt techniques for life stages and health needs. Gentle, low-force methods are available, and we coordinate with your other providers when appropriate.
TL;DR Summary
- Stress can trigger headaches by tightening neck/shoulder muscles, altering posture, and sensitizing the nervous system.
- Tension-type and neck-related headaches are most commonly linked with stress; migraines can be stress-triggered too.
- Chiropractic care addresses joint mobility, muscle tension, posture, and habits—often reducing frequency or intensity.
- Simple routines—movement breaks, hydration, sleep, and breathing—support long-term relief.
- Seek urgent medical care for sudden severe headache, neurological changes, fever with neck stiffness, or after head injury.